KDI FOCUS Building a New Safety Net for Sick Workers June 28, 2022
Building a New Safety Net for Sick Workers
June 28, 2022
The effective rollout of the Sickness Benefits as a social safety net for sick workers hinges on sick leave readily accessible in the workplace. To that end, sickness benefits should include assistance for firms vulnerable to extra costs incurred by sick leave. Also, the level of sickness benefits should be differentiated based on the duration and severity of illness or injury. To ensure the sustainability of Sickness Benefits, the scheme further requires measures to strengthen medical certification and to support workers’ return to work after a spell of sick leave.
Ⅰ. New Safety Net and Challenges to Its Adoption
Sickness benefits are a safety net providing income support to workers who are unable to work due to an illness or injury. With COVID-19 came an awareness that sick leave is essential for individual health and the well-being of society and growing demand for sickness benefits as a new safety net. In response to the emerging social demand, the Korean government is
pushing to introduce a model for sickness benefits.
However, its pilot project launching in July 2022 seems to fall short in effectiveness as a safety net for sick workers. First, while the receipt of sickness benefits is predicated on workers getting rest when unwell, the pilot model only makes up for the income loss for the days incapacitated to work, without guaranteeing a sick leave. Due to the lack of guaranteed sick leave, vulnerable workers, who already face constraints in taking leave, may have lower accessibility to the
In the aftermath of COVID-19, Korea is pushing for a homegrown model of sickness benefits, but its scheduled pilot project seems to fall short as an effective safety net for sick workers.
system. Second, the model provides a flat rate of 60% of the 2022 minimum wage (43,960 won per day) up to 90 days, or 120 days, irrespective of the severity of illness. Due to the low level of benefits, the current model has limited effectiveness as an income safety net for workers at a higher risk of diseases or injuries. Third, the pilot program lacks sufficient strategies for
controlling the unnecessary receipt of sickness benefits.
A pilot program helps estimate the program's impact on a large-scale and redress issues to improve policy effectiveness once fully launched. For the sickness benefit model to deliver adequate protection for sick workers and ensure sustainability, this study examines components worth considering for future pilot programs, suggesting policy directions for establishing the new safety net.
II. Benefit Gap and the Possibility of Dual Operation
1. Gap in Sick Leave Eligibility
Short-term and long-term sick leave of absence should be guaranteed for workers to take time off work when they are sick. Without such guarantees at workplaces, sick workers have to take personal or unpaid leave. In Korea, the Labor Standard Act does not stipulate suspension from work for reasons of non-occupational injury or disease, and sick leaves, paid or unpaid, are regulated mainly by collective bargaining agreements or employment rules at the firm level. A limited number of business establishments sign collective agreements, which may not be applicable depending on the type of employment. As a result, only a small share of workers are entitled to use sick leaves when needed.
For the sickness benefit scheme to operate effectively, it is crucial to have institutional backing that allows workers to take time off work, such as short-term and longterm sick leave.
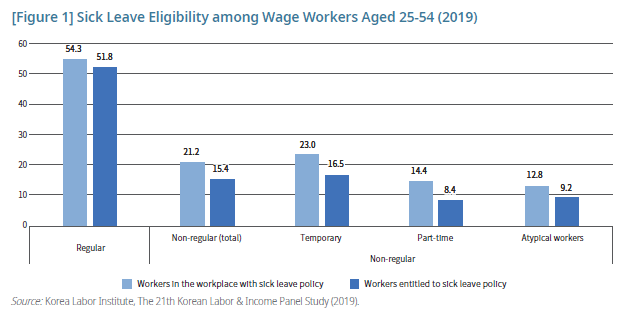
[Figure 1] shows sick leave eligibility of wage workers, sorted by employment status. Of wage workers in their prime working age (25~54 yrs), 45.5% are working in jobs that provide sick leave, and 42.1% are entitled, which is less than half of the total prime working-age population. Even for regular employees, the share of those with employee sick leave policies in place at work is 54.3%, implying weak safety nets for sick workers regardless of job security and stability. Non-regular workers are in an even more vulnerable situation. 21.2% have a sick leave policy at work, and a mere 15.4% are entitled to the benefit. Eligibility for sick leave differs according to the job security. Of atypical workers, including dispatch, subcontract, and daily workers, only 9.2% are covered by firms’ sick leave policies.
The size of business establishments is a major determinant of job quality, and another eligibility gap is found between firms of different sizes in Korea (Figure 2). Of workers in establishments with 300+ employees, 66.4% are entitled to sick leave, while only 21.4% in small-sized establishments with fewer than 30 employees. In small firms, only 28.5% of regular workers and 7.1% of non-regular workers have the option of sick leave. As of 2019, those working in small companies account for 47.3% of the total number of workers, and 25.9% are in much smaller ones with fewer than five employees without annual leaves guaranteed under the Labor Standards Act. Given these figures, even after adopting the sickness benefit package, a considerable portion of workers may continue to have difficulties receiving the benefit (Statistics Korea, Dec. 3, 2020).
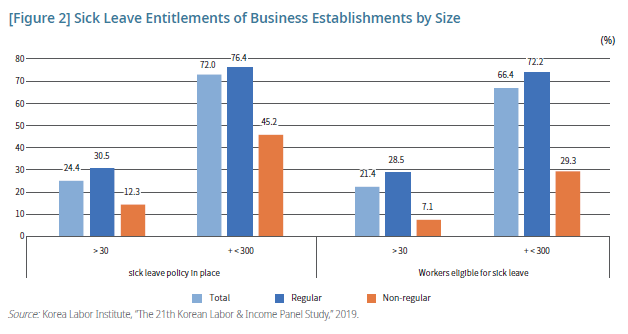
Of regular workers in business establishments with 300+ employees, 72.2% are eligible for sick leave, contrary to only 7.1% for nonregular workers in businesses with fewer than 30 employees. This finding indicates a considerable gap in sick leave entitlements among workplaces of different sizes and job security.
The Korean sickness benefit model is built on the foundation of universality, inclusive of all working people (Kang, 2021). However, even with the benefit system established as a universal safety net, many workers whose entitlements to sick leave are not guaranteed may still be exposed to the risk of job loss during sickness absence spells. The insufficient protection for the
most vulnerable workers may beget another problem of uneven benefits between workers who can and cannot use sick leave.
2. Gaps in Health Status and Work Environment
The health status of workers, as well as unsafe work environments affecting health, have a direct impact on the demand for sickness benefits. Given the access gap to sick leave between jobs, a further divide in health may exacerbate inequities in access to sickness benefits, especially for those with greater needs. This study uses the Korean Working Conditions Survey to examine health status indicators of full-time, prime-age (25~54 yrs) wage workers by employment status. It found a clear difference in health status between workers according to their employment stability proxied by employment status (Table 1).
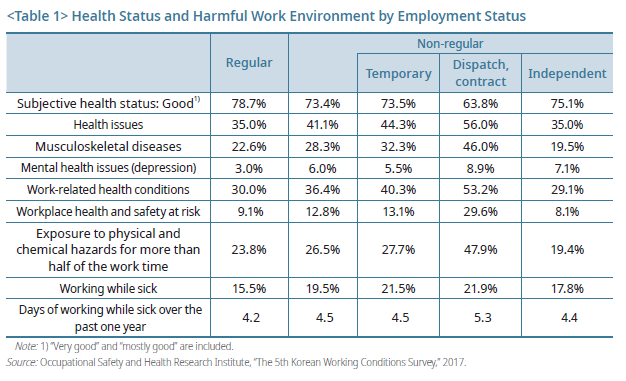
Amidst the disparity in accessibility to sick leave, there exists a health gap between regular and nonregular workers, and the systemic health divide goes further among non-regular workers by contract types.
Multiple health indicators have shown that non-regular workers are in poorer health than regular workers, and non-regular workers exhibit systematic differences by employment subtypes within the group (Table 1). This divide between regular and non-regular employment is seen in subjective health status on overall health conditions independent of the actual incidence of diseases and the occurrence of health problems such as chronic illness. Among non-regular workers, dispatch and subcontract workers rank the lowest in subjective health status and the highest in the occurrence of health problems.
Exposure to harmful working conditions with potential negative health impacts shows systematic disparities depending on employment type.
Countries with sophisticated sickness benefit systems have faced the issue of frequent and long-term claims of musculoskeletal diseases. Korea is likely to see a rapid payout increase after adopting the package due to musculoskeletal conditions since they are also quite common among Korean workers. In particular, dispatch and subcontract workers with relatively poor health have a share of 46% suffering from musculoskeletal pain. Such a high figure has to do with the fact that many of them are engaged in labor-intensive jobs, like elementary occupations related to cleaning and protective services (18.1%) and construction and mining (14.8%), and their average age is relatively higher than those in other occupations.
The disparity in exposure rates to hazardous working conditions that can have adverse effects on health remains persistent between regular and non-regular workers. Of non-regular workers, dispatch and subcontract workers are at a much greater risk than others. As for whether their work involves risks to their health and safety, 9.1% and 12.8% of regular and nonregular workers, respectively, said yes, while of non-regular workers, 29.6% of dispatch and subcontract workers said yes.
Given the association between a dangerous work environment and occupational diseases or injuries, it may seem that hazardous working conditions are unrelated to adopting sickness benefits that are a safety net for non-occupational illnesses or injuries. However, working conditions are a key determinant of health inequality among workers (Benach et al. , 2014). Moreover, it is hard to rule out the possibility that diseases or injuries caused by precarious work conditions fall into the scope of the benefit coverage. The followings are taken into account to make such a deduction: difficulty in proving strict causality between work and illness; complexity in specifying employers due to the growing diversity of employment types; and a tight correlation between sicknesses that are occupational and non-occupational, as in Spain's case that claims for work-related diseases and injuries increased after tightening eligibility conditions for sickness benefits (Marie and Castello, 2020). Hence, improving unsafe work environments does matter as a means to proactively manage working conditions liable for increased demand for sickness benefits. In the mid-to-long term, it is desirable to take an approach that ensures the benefits scheme lives on as preventive measures.
For sickness benefits to effectively protect vulnerable workers,the establishment of a sick leave system and the improvement of workers’ health and working environment are necessary.
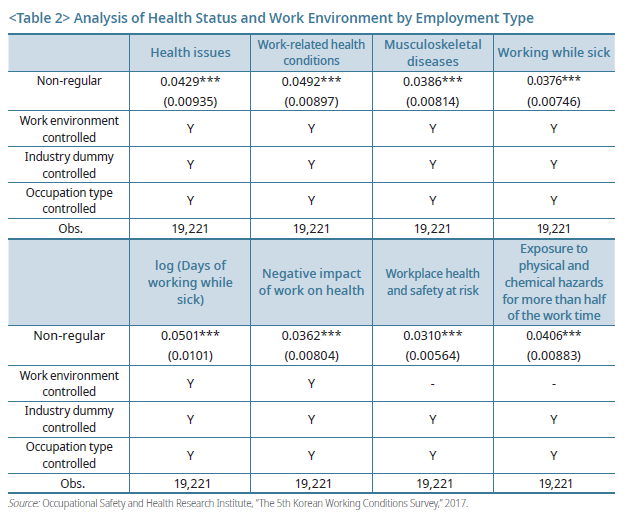
In addition, presenteeism is more common for non-regular workers than their peers with permanent contracts. Rates of presenteeism are 15.5% for regular workers and 19.6% for nonregular workers. Also, the number of days worked when sick is higher in non-regular workers than in regular workers. Within the category of non-regular workers, dispatch and subcontract workers with poorer health and more exposure to hazardous work conditions reported the highest number of days worked when sick, with 5.3 days per year. In an empirical analysis controlling for individual characteristics and job characteristics, non-regular workers were found to have poorer health conditions and frequent exposure to hazardous working environments compared to regular workers. The prevalence of presenteeism is also meaningfully high among non-regular workers.
For wage workers, health status, harmful working conditions, and safety nets differ greatly depending on employment stability, and job quality. Workers with less access to sick leave, in particular, are more likely to be less healthy, more exposed to harmful working conditions, and exhibit presenteeism. That is, the inequality can lead to an irony that workers most needing the benefits face greater challenges in receiving the benefits. Consequently, for sickness benefits to effectively protect vulnerable workers on the outskirts of the scheme, the establishment of a sick leave system and the improvement of workers’ health and working environment are necessary, in addition to guaranteeing lost income. Also, special attention should be given to jobs with high health risks by reducing hazardous factors in each industry and occupation.
III. Changes in Employment and Income Facing Sick Workers
This section examines essential components of sickness benefits that merit our attention when designing the policy. We discuss the necessity of such benefits based on an empirical analysis of the extent of changes in employment and income of workers incurred by illnesses.
1. The Need for Safety Nets in Job and Income for Sick Workers
상First looked at are the changes in employment and income of workers who had to discontinue work for a certain period due to sickness. Hospitalization validates workers' inability to work for a certain period, hence defining it as grounds to suspend working in a bout of illness. Samples are full-time wage workers in their prime working age (25-54 yrs) who have been employed for at least two years. The analysis examines the impact of three or more days of continued hospitalization (hospital-level or higher) on their medical expense, employment, and income.
분According to the analysis, sick workers’ medical expenses increased only during hospitalization, but their employment remained affected not just during the year of hospitalization but beyond it. In the year of hospitalization, the labor force participation rate decreased by 3.8%, compared to those without such experience, followed by continued decreases of 7.4% after one year and 9.2% after two years. The probability of continuing fulltime wage work also decreases by 6.6% in the year of hospitalization, 11.6% after one year, and 12.3% after two years.
The declining labor participation after hospitalization leads to reduced labor income (Figure 4). In the year of hospitalization, the labor income decreased by 24.2%, compared to individuals without the experience of hospitalization, followed by 40.7% after one year and 44.5% after two years. On the other hand, no significant decrease in income is observed in individuals who returned to full-time work or at least stayed in the labor market after hospitalization, except for in the year of hospitalization. A continued decline in income appears mostly among individuals who lost jobs.
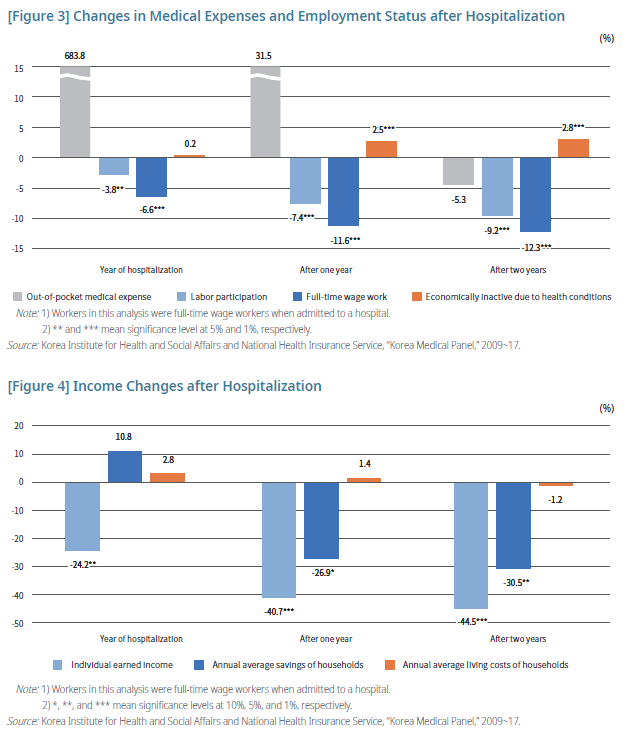
Workers with the experience of hospitalization, which defines health shock in this study, are found to experience a continued decline in their employment and income afterward.
Job loss from sickness or family caregiving takes significantly longer until reemployment than other involuntary job losses (Kwon, 2021b). Getting back to work is particularly difficult for workers who have been sick, unlike other displacements in which job seeking is possible right away. It is because job search can begin only after recovering from productivity loss caused by ill health. Besides, finding a job that can accommodate personal health issues in terms of work intensity and conditions is never easy. Displaced sick workers with difficulties getting back into work often suffer from reduced earnings. As a result, short-term income support has limited effects, suggesting that the assistance for sick workers needs to focus on helping them remain connected to the labor market.
In particular, a prolonged decline in earnings is most pronounced among displaced workers by sickness, which suggests the need to support them to remain connected to the labor market, coupled with financial assistance.
The annual average living costs of households do not show any significant difference between before and after hospitalization. Household savings, in contrast, are found to decrease by 26-30% after one year. Such patterns suggest that households experiencing a loss in labor income due to the health conditions of their member are using savings to smoothen consumption. This finding of a sustained level of consumption in households hit by a health shock might cast doubt on the effectiveness of sickness benefits. However, arriving at this conclusion needs careful consideration. First, this analysis covers individual wage earners who retained a full-time job for more than two years at the same workplace. They are relatively stable employees and more likely to be capable of consumption smoothing with assets like savings at their disposal, compared to the average of all wage earners. Second, even when their behavior can be explained as a consumption smoothing response, their use of various or inefficient means in the process will likely bring in large welfare gains when the sickness benefit system is adopted (Chetty and Looney, 2006).
The results imply that expanding support confined to medical expenses, for instance, by strengthening health insurance coverage and emergency subsidy for disaster medical costs, does not provide enough safety nets. It also demonstrates the need for the sickness benefit package as a safety net to compensate for the earnings losses of sick workers who had to discontinue working for some time. Furthermore, since the leading cause of income reduction for these workers is job displacement from sickness, sick benefits by design should include specific programs for their employment stability, such as assistance to ensure job retention and return-to-work.
2. The Need for Differential Income Replacement Ratios
This section presents an analysis of the changes in employment and income by hospitalization period and types of inpatient medical facilities, both closely related to the severity of sickness, followed by discussions on specific policy design of sickness benefits based on workers’ health status. The severity of an illness or injury chiefly determines the period of inability to work and the possibility of a return to work, which may result in different levels of wage loss. The waiting period is the extent of time from the occurrence of illness to the onset of receiving benefits, and it serves as a means to control imprudent benefit provision. The typical waiting period for the sickness benefit is between three and seven days.The analysis examines the impact of the length of hospitalization, three to seven days or longer, on employment and income.
The results find no significant decrease in employment and income for those who experienced short-term hospitalization (3~7 days), except for some declines in labor force participation one year later. On the other hand, for a more extended stay at hospitals (8+ days), the likelihood to keep working full-time beginning from the year of hospitalization decreased by more than 5% compared to those without hospitalization, and their earnings also shrank by more than 35%. Such results suggest that given limited financial resources, strengthening support for long-term health impairments instead of short-term diseases or injuries may be a more effective safety net for workers suffering from earning shocks.
As workers experience varying impacts on their employment and income depending on the severity of sickness, the benefit coverage for those suffering from serious diseases needs to be further expanded for safety nets to provide more practical support.
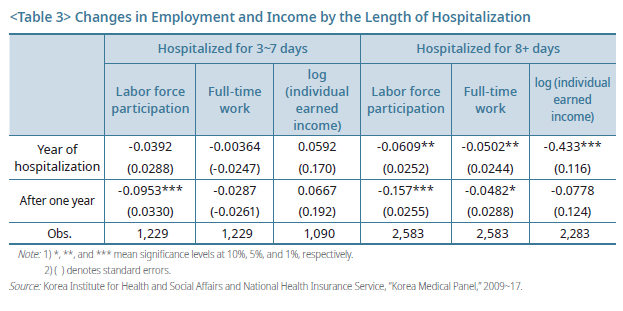
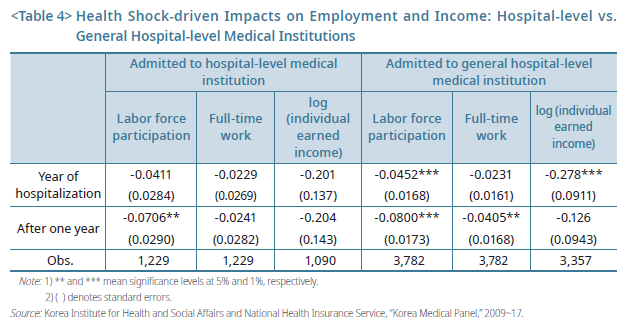
In another analysis, types of hospitals such as hospitals and general hospitals and above, were used as proxies for the severity of sickness to look into the impact of hospitalization on workers' employment and income. While the level of hospitals cannot be precisely equivalent to the illness severity, the higher up the tiers, the greater share of the severely ill can be expected. Accordingly, it finds no explicit decline in employment and income among workers admitted to hospital-level institutions due to relatively less severe sickness but a clear decline among those in general hospital-level or higher institutions (Table 4).
The two findings hint at what makes safety nets more effective. Instead of a comprehensive support scheme that includes minor illnesses with less adverse effects, it should broaden the coverage of sickness benefits to capture long-term injuries or severe diseases with clear negative impacts on employment and income.
IV. Policy Recommendations
1. Statutory Sick Leave and Support for Vulnerable Businesses
As the Korean design of sickness benefits builds on its national health insurance, the systemic blindspot generated by the employment insurance scheme is relatively limited. Nevertheless, the current policy design that fails to guarantee sick leaves may create a substantial blindspot that denies intended policy recipients the entitled access in practice. Hence, unpaid sick leave should be made a statutory holiday to guarantee access to sick leave with pay, even in the workplace that does not accommodate them, for the benefits scheme to serve as a universal safety net.
While improving the receptivity of employers by providing financial assistance to employment costs incurred by its adoption, unpaid sick leave, at least, should be made into law to prevent the sickness benefit scheme from operating in two modes.
However, enhancing its effectiveness through sick leave legislation may lead to higher employment costs for small businesses without a sick leave policy. Notably, the extra workload of other workers and the employer's burden of filling vacancies resulting from absences lead to reluctance for employers to adopt sickness benefits. Thus, policy efforts should help create favorable soil for the new system by reducing the hiring burden of easily affected businesses. Such measures can consult subsidies for hiring new or replacement workers like the employment stabilization program for maternity and parental care, given the similar intent to provide support for additional employment costs arising from adopting a new scheme. In addition, conducting and evaluating the pilot project should be accompanied by closely examining the frequency of benefit spells and the cost amount incurred for businesses with and without the sickness package. Based on the results, the second phase of this project should include specific plans to have the sick leave system firmly established and support small businesses in the adoption process.
Repeated receipt of sickness benefits for shortterm minor sicknesses should be discouraged by applying different income replacement ratios per the severity of illness. At the same time, long-term severe diseases should receive more robust protection in the safety net.
2. Sickness Benefits Differentiated by the Severity of Sickness
The pilot sets a low fixed amount of 43,960 won per day for sick pay, dispensed evenly throughout work disability duration due to illnesses or injuries. However, the probability of job retention and the extent of income reduction display significant variations depending on the length and severity of sickness. Consequently, effectively safeguarding the health of workers exposed to a greater risk under limited resources requires a policy design that differentiates the safety net's protection level subject to the severeness. Additionally, sickness benefits should provide further protection for severe long-term sickness with a more extensive adverse impact on employment and income and a narrower coverage for short-term health issues with a lower risk of job loss and earnings decline.
In most countries that have instituted sickness benefit schemes, sick pay is defined by the income replacement ratio and the level is around 38~100% of the income before the incidence of sickness. Countries with stable sickness benefit systems, including Sweden, Germany, and Spain, have reformed them since the 1990s by applying differential replacement ratios based on the length of sick leave, which assigns higher ratios for long-term illnesses. Such reforms aim to control the unnecessary use of the benefits by raising the opportunity cost of benefits spells for minor illnesses over the short term while providing a sufficient safety net for long-term severe diseases.
Stringent medical certification is required to mitigate the moral hazards of sickness benefits.
In the early adoption phase, granting large benefits is hard to achieve. The first phase of the pilot program provides benefits at a flat rate in line with the primary objective of evaluating the frequency of sickness benefit spells; however, the benefits should vary per illness duration before bringing it to full scale. To that end, the next pilot design needs an additional component for evaluating the effectiveness of safety nets and changing behavioral patterns after receiving the different benefits depending on the length of healthcare and recovery.
The benefit scheme should add workability evaluation in its medical certification to move toward an active labor market policy that promotes returning to work.
3. Medical Certification and Support to Return to Work
Prolonging the waiting period and differentiating income replacement ratios per sickness duration may cause moral hazards, such as increased indiscriminate use of medical services for collecting sickness benefits. Accordingly, medical certification verifying benefit eligibility should be more stringent to control unnecessary usage. Also, the certificate system in its design should support returning to work and furnish a job-specific workability evaluation.
Unfettered by passive income guarantees, support for return-to-work should take up an active policy that links work and welfare. The ultimate goal of sickness benefit is more than guaranteeing earnings. It is also to help sick workers restore labor productivity and retain employment by ensuring their right to rest in a bout of illness and compensating for wages lost to sickness. As such, there is a need to prevent sick workers' permanent dismissal from the labor market by incorporating the active labor market policy into the sickness benefit system. To that end, the system should be furnished with a mechanism to control the incentives to succumb to moral hazards in the early stage of adoption by design. Together with details on benefit payments and spells, it is desirable to include evaluations of benefit eligibility and workability as well as return-to-work assistance. Initially, assessing health status and return-towork readiness may be costly, but these measures can improve sustainability in the long run.
Furthermore, unlike regular health checkups, the readiness to return to work should be evaluated based on the work environment and conditions specific to returning workers. Also, in terms of the heavy workload and the legitimacy of evaluation, it is problematic for general medical institutions to carry out workability evaluations even with the exclusive responsibility for medical certification to the National Health Insurance Service. Therefore, measures for follow-up management are needed to conduct medical checkups on benefit recipients before returning to work, arrange job placement and transfer, and address workplace-specific health issues.
< sources >Korea Institute for Health and Social Affairs and National Health Insurance Service, “Korea Medical Panel,” 2009~17.
Korea Labor Institute, “The 21th Korean Labor & Income Panel Study,” 2019.
Occupational Safety and Health Research Institute, “The 5th Korean Working Conditions Survey,” 2017.
CONTENTS-
- Ⅰ. New Safety Net and Challenges to Its Adoption
Ⅱ. Benefit Gap and the Possibility of Dual Operation
Ⅲ. Changes in Employment and Income Facing Sick Workers
Ⅳ. Policy Recommendations
- Ⅰ. New Safety Net and Challenges to Its Adoption
- Key related materials
We reject unauthorized collection of email addresses posted on our website by using email address collecting programs or other technical devices. To access the email address, please type in the characters exactly as they appear in the box below.
Please enter the security code to prevent unauthorized information collection.

